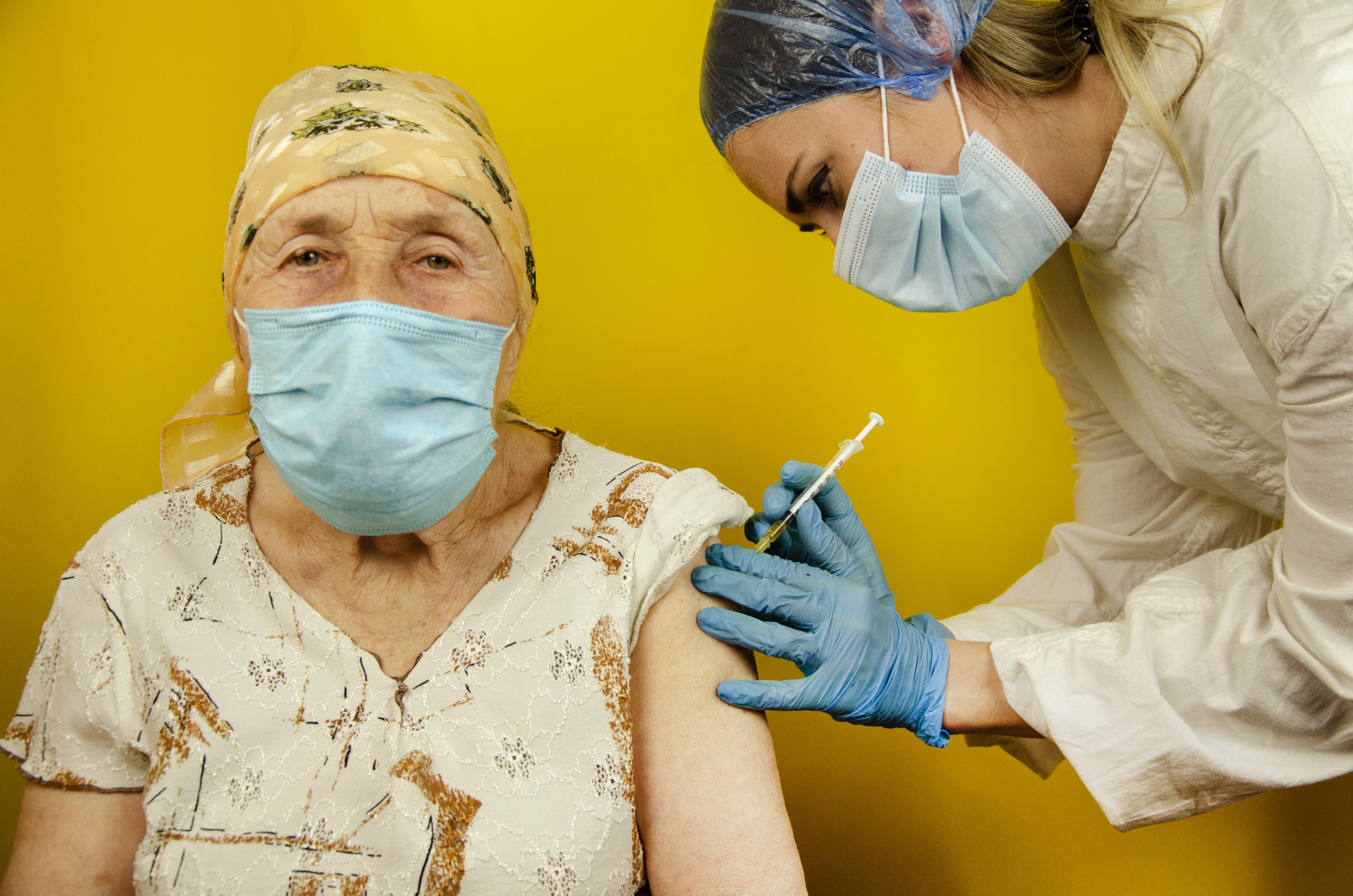
Looking at declining immunity especially among nursing home residents
Brown
University
To address the pressing issue of diminishing immunity among older adults to COVID-19 as well to vaccines designed to protect against the virus, a $4.9 million award from the U.S. Centers for Disease Control and Prevention will fund a two-year project led by Brown University researchers and conducted by a team spanning multiple institutions.
The
researchers will examine the duration of protective immunity in the context of
emerging strains of COVID-19, releasing interim data to the CDC as it becomes
available to inform policy decisions in real time.
“Given
rising case counts of the Delta variant, we need to know as soon as possible
who needs a vaccine booster shot and when they need it,” said Stefan
Gravenstein, co-lead investigator on the project and a professor of geriatric
medicine at Brown. “This information on how specific immunity to SARS-CoV-2
infection declines with aging, disease and in long-term care residents is
critically important for developing a booster strategy based on real-time data
in this population.”
The CDC awarded the contract to Gravenstein; Elizabeth White, a Brown assistant professor of health services, policy and practice; and David Canaday at Case Western Reserve University. The project is based at Brown’s Center for Long-Term Care Quality and Innovation, which focuses on research to improve care and quality of life for older adults living in nursing homes.
The
new award builds on previous research about
protective immunity over time conducted by Gravenstein and Canady. Their most
recent study, published online in
late August, found that COVID-19 antibodies produced by the Pfizer vaccine
decreased sharply in nursing home residents and health care workers six months
after receiving their second shots.
For that study, the research team studied blood samples of 120 nursing home residents and 92 health care workers. In particular, they looked at humoral immunity — also called antibody-mediated immunity — to measure the body’s defenses against the coronavirus.
The researchers, including a lab team at
Harvard University, found that individuals’ antibody levels decreased more than
80% after six months; the decline was similar in residents (median age 76) and
health care workers (median age 48), according to the study. However, absolute
antibody levels were much lower in the nursing home residents who had not also
had a prior infection than the comparison groups.
After
presenting their unpublished results directly to senior staff at the CDC, the
researchers were urged to get the data out in the public domain as soon as possible
to inform the decision-making process for booster vaccine recommendations. As a
result, the researchers published the findings as a preliminary report ahead of
peer review on medRxiv,
an online preprint server for health sciences studies co-founded by Cold Spring
Harbor Laboratory, Yale University and the BMJ, a global healthcare knowledge
provider. The study is currently under review at a traditional peer-reviewed journal.
Another
study by Gravenstein, Canaday and colleagues published
last May found that within two weeks of receiving the second
dose of vaccine and being considered “fully vaccinated,” seniors who had not
previously contracted the virus that causes COVID-19 mounted a substantially
lower response to vaccine than experienced by younger health care workers. By
six months after vaccination, 70% of these nursing home residents had blood test
results showing a poor ability to neutralize the virus.
The
preprint research is useful as the team continues to examine immunity in
elderly patients.
“Aside
from the obvious value of better understanding who and when to boost against
SARS-CoV-2 infection, we’ve also substantially innovated in how to efficiently
recruit and immunologically follow a long-term care population,” Gravenstein
said. “This methodological advancement leverages Brown’s strengths in the
intersection between biology, aging and public health research.”
Results up to this point support the CDC’s recommendation for booster shots — especially for the elderly — due to fading immunity, Gravenstein said.
The team
will now study 800 to 1,200 nursing home residents who have received one of the
SARS-CoV-2 vaccines or who will newly receive a vaccine or booster, if and when
boosters are federally recommended, and will assess their overall health and
immune responses to see whether and how immunity to COVID changes over time.
The team will continue to produce and share data in six-month segments.
As
older residents in the study become re-vaccinated, Gravenstein said, this work
will show whether that vaccination bolsters not just antibody levels and
immediate protection, but also fortifies more durable defenses against new,
incoming strains.
COVID-19
isn’t going away, Gravenstein said — if anything, it’s becoming more like the
flu in its persistency, and as the virus becomes more endemic to modern
society, “this information on immunity will be critical to know.”