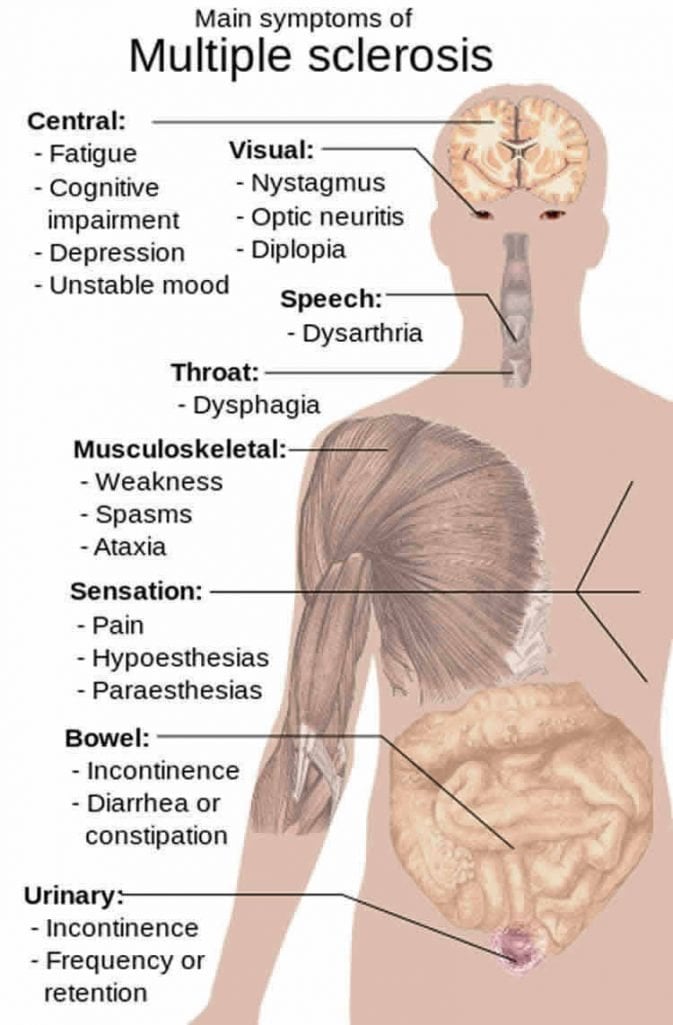
A good reason to curb your salt use
By Kevin Dennehy, Yale University
The connection between salt consumption and autoimmune diseases has been clarified by a Yale-led study, which found that elevated salt levels contribute to the dysfunction of regulatory T cells through the overexpression of the protein PRDM1-S, suggesting new treatment pathways for conditions like multiple sclerosis.Researchers at Yale have identified a protein that triggers
loss of immune regulation associated with multiple sclerosis and other
diseases.
This discovery, which highlights the role of
environmental factors like high salt intake, offers a new target for developing
universal autoimmune treatments.
Groundbreaking Discoveries in Autoimmune Research
More than two decades ago, a research team in the lab of
David Hafler, a Yale researcher who at the time was at Harvard, discovered a
type of T cell in humans that suppresses the immune system; they later found
that these so-called regulatory T cells, when defective, are an underlying
cause of autoimmune disease, specifically multiple sclerosis (MS). For many
years, however, the mechanism behind this dysfunction has remained unclear.
In a new Yale-led study, a team of researchers finds that
this loss of immune regulation is triggered by an increase in PRDM1-S, a
protein involved in immune function, triggering a dynamic interaction of
multiple genetic and environmental factors, including high salt uptake.
The findings, published on August 28 in the journal Science Translational Medicine, also reveal a new target for a universal treatment for human autoimmune disease.
The research was led by Tomokazu Sumida, an assistant
professor at Yale School of Medicine (YSM), and Hafler, the William S. and Lois
Stiles Edgerly Professor of Neurology and professor of immunobiology at Yale.
Unveiling the Mechanism of MS
“These experiments reveal a key underlying mechanism for the
loss of immune regulation in MS and likely other autoimmune diseases,” said
Hafler, who is also chair of Yale’s Department of Neurology. “They also add
mechanistic insight into how Treg [regulatory T cells] dysfunction occurs in
human autoimmune diseases.”
Autoimmune diseases, among the most common disorders of young adults, are known to be affected by genetic and environmental factors, including vitamin D deficiency and fatty acids. In an earlier study, Sumida and Hafler found that high levels of salt also contribute to the development of multiple sclerosis, an autoimmune disease of the central nervous system.
Specifically, they observed that high salt induces inflammation in a type of immune cell known as CD4 T cells, while also causing a loss of regulatory T cell function. This, they found, is mediated by a salt-sensitive kinase, or enzyme critical for cell signaling, known as SGK-1.
For the new study, researchers used RNA sequencing
to compare gene expression in patients with MS with expression in healthy
individuals. In patients with MS, the researchers identified upregulation, or
increased expression, of a gene called PRDM1-S (primate-specific transcription
factor), also known as BLIMP-1, which is involved in regulating immune
function.
New Potential Targets for Autoimmune Treatments
Surprisingly, PRDM1-S induced increased expression of the
salt-sensitive SGK-1 enzyme, leading to disruption of regulatory T cells, the
researchers found. Moreover, they found similar overexpression of PRDM1-S in
other autoimmune diseases, suggesting that it may be a common feature of
regulatory T cell dysfunction.
“Based on these insights, we are now developing drugs that
can target and decrease expression of PRDM1-S in regulatory T cells,” Sumida
said. “And we have initiated collaborations with other Yale researchers using
novel computational methods to increase the function of regulatory T cells to
develop new approaches that will work across human autoimmune diseases.”
Reference: “An autoimmune transcriptional circuit drives
FOXP3+ regulatory T cell dysfunction” by Tomokazu S. Sumida, Matthew R.
Lincoln, Liang He, Yongjin Park, Mineto Ota, Akiko Oguchi, Raku Son, Alice Yi,
Helen A. Stillwell, Greta A. Leissa, Keishi Fujio, Yasuhiro Murakawa, Alexander
M. Kulminski, Charles B. Epstein, Bradley E. Bernstein, Manolis Kellis and
David A. Hafler, 28 August 2024, Science Translational Medicine.
DOI:
10.1126/scitranslmed.adp1720
The study was done with Bradley Bernstein and Manolis
Kellis, longtime collaborators of Hafler from the Broad Institute of MIT and
Harvard, and several other research institutions.
Other authors from the Yale lab include neurologist Matthew
R. Lincoln, and post-graduate research assistants Alice Yi, Helen Stillwell,
and Greta Leissa.